Solutions

MDsyncNET’s cloud-based software reduces inefficiencies, delivers immediate results, and maximizes ROI.
WHO WE SERVE

MDsyncNET delivers right-sized software to healthcare organizations in a variety of environments.

While the COVID-19 pandemic has taken a toll on every person living on Planet Earth, none have felt the impact more keenly than frontline healthcare workers. A year into the pandemic, The Guardian reported that more than 3,600 U.S. healthcare workers had lost their lives to the novel coronavirus. More than half were younger than 60, a majority were people of color, and one in three were nurses.
Unfortunately, the tragically high number of nurses who have sacrificed their lives caring for COVID-19 patients is just one factor fueling a nursing crisis in the U.S. In late summer 2021, the New York Times reported that nursing shortages had reached catastrophic proportions. While exact numbers are elusive, the U.S. Bureau of Labor Statistics estimated that more than 3 million nurses were employed in 2020, and that there would be 9 percent job growth over the next decade. But then COVID-19 hit. Now, it’s estimated that up to 1 million nurses could retire by 2030. Faced with never-ending shifts, an avalanche of younger and sicker unvaccinated patients, and the possibility of care rationing, it’s unsurprising that many hospital nurses are opting for retirement or positions in other, less stressful environments.
The critical nursing shortage is marching in lockstep with a growing unease among the broader swath of healthcare workers. A survey conducted by the Washington Post and Kaiser Family Foundation found that more than half of frontline workers are burned out and 29 percent have considered leaving healthcare altogether.
Hospital staffing shortages are exacerbated when workers refuse to comply with vaccine mandates. Reuters reported that New York’s Governor is considering declaring a state of emergency, which would pave the way to bring in healthcare workers from other states and deploy the National Guard to boost staffing at medical facilities across the state. In August, Oregon’s governor ordered 1,500 National Guard troops to help staff hospitals. The Guardian reported that the federal government has sent more than 350 healthcare professionals to shore up hospital staffing in Louisiana, Mississippi, and Alabama.
These staffing shortages are having devastating impacts on both patient care and hospital revenue streams. The lack of nurses has meant that hospital beds remain empty while emergency departments are drowning. Overwhelmed emergency departments are forced to turn away patients who don’t have COVID, but who instead are presenting with everything from heart attacks to strokes to gunshot wounds. States including Idaho and Alaska have implemented crisis care standards, meaning that physicians and hospital committees are put in the excruciating position of deciding which patients are most deserving of care and which are not. Many hospitals are refusing patients who need care from specialists, robbing patients of care and organizations of significant revenue. In addition, elective and non-emergent surgeries are again on hold at many facilities, negatively impacting revenue.
Hospital schedulers had their hands full prior to the pandemic. Now, they’re like air traffic controllers at O’Hare over Thanksgiving weekend. But, while air traffic controllers have the latest technology at their fingertips, schedulers often are stuck with spreadsheets or pen-and-paper.
Pre-COVID, manual physician scheduling processes led to myriad problems. The wrong on-call physician might be contacted. Outdated schedules could cause confusion. And each traded shift necessitated creating and distributing an updated schedule.
Today’s scheduling is exponentially more complicated. Physicians, nurses, and other clinicians may become suddenly unavailable due to COVID-19 quarantine or illness. Shift length and the number of shifts per week may increase. Competition among hospitals for nurses may result in a high degree of turnover. And, according to a Washington Post report, the mental and physical toll of caring for COVID-19 patients can cause healthcare team members to simply walk off the job. The result? Scheduling becomes a balancing act of trying to do more with less.
On the other side of the scheduling equation is the influx of new staff members from disparate sources. The roster of healthcare professionals may surge when locum tenens doctors, traveling nurses, National Guard troops, or out-of-state practitioners show up. Surge scheduling is all the more challenging when the hospital census fluctuates from day to day.
While healthcare scheduling software can’t solve the COVID-19 pandemic, it can solve the resulting scheduling crisis. Cloud-based scheduling is nimble, able to adapt to expansion and contraction of available staff. Real-time scheduling updates are easy to implement, and the resulting up-to-the-minute schedules are accessible via mobile app or web browser. This single source of truth ensures that every member of the healthcare team is in sync, alleviating the avoidable stress of unpredictable scheduling changes.
Using historical data gathered from after World War II, the SARS epidemic, and the 2008 financial crisis, McKinsey & Company noted, that public companies that innovate through a crisis outpace their peers in economic growth. Implementing healthcare scheduling software as a solution is an innovation that can strengthen healthcare organizations’ infrastructure during and beyond the era of COVID-19.
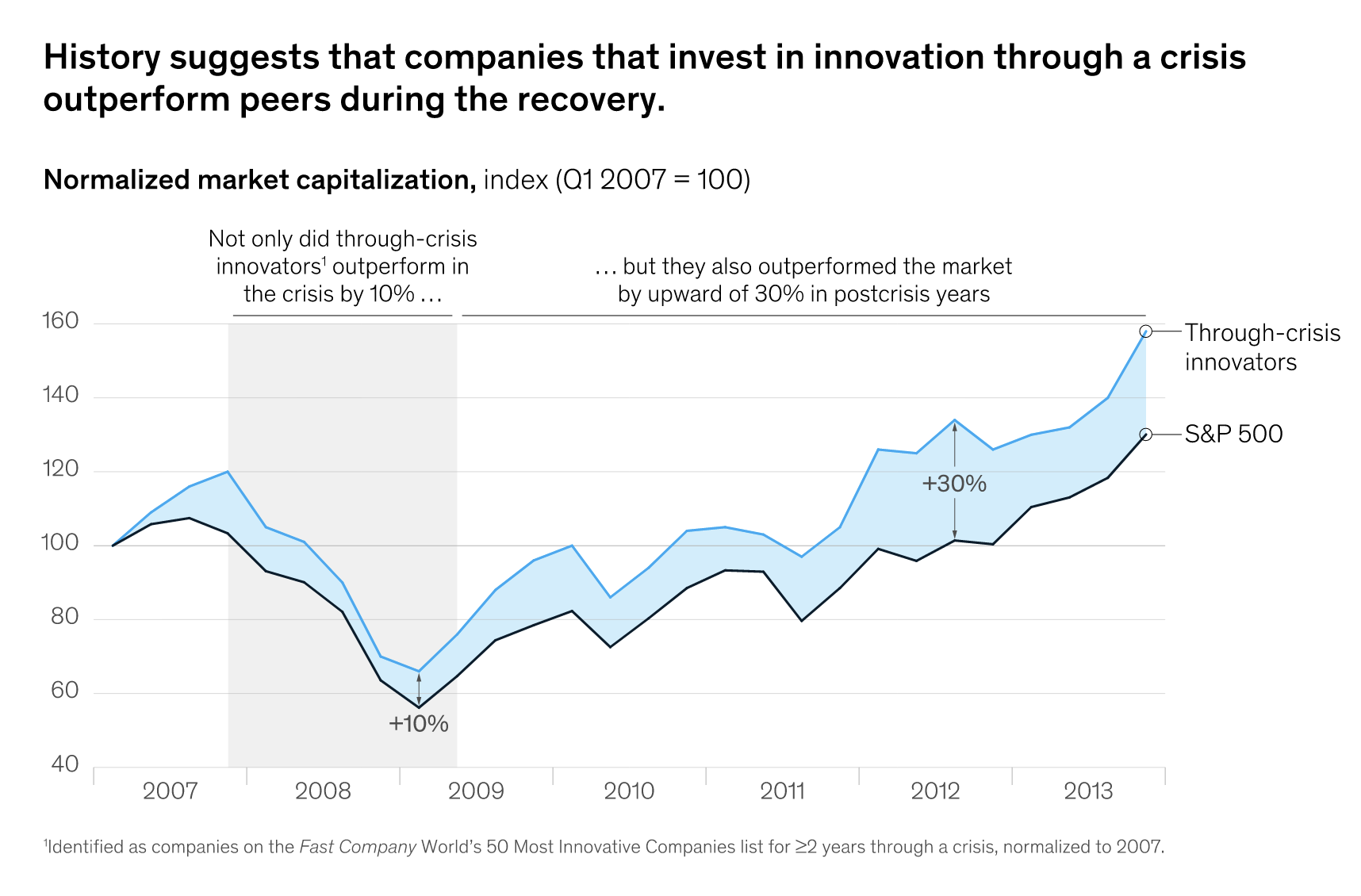
Chart by McKinsey & Company
Healthcare scheduling software can do the heavy lifting as hospitals navigate staffing shortages and surges. It supports patient safety, enhances scheduling productivity, and contributes to the bottom line. Most of all, it supports frontline healthcare workers who need all the help they can get during the COVID-19 pandemic and beyond.
MDsyncNET’s cloud-based healthcare scheduling software is affordable, simple to learn, easy to use, and has a 98% adoption rate across hospital systems. To learn more about the MDsyncNET advantage, visit MDsyncNET.com or call 888-506-5061.

© 2022 All Rights Reserved. MDSYNCNET | Privacy Policy & Terms and Conditions